We’re all taught in school how the brain makes up the most important part of the body. But even the brain can’t survive without the heart to keep the blood flowing, to bring it oxygen. That only goes to show just how important the heart is. Your heart is the center of your cardiovascular system, and it is responsible for nearly everything that keeps your body alive and healthy. Out of all the facts about the heart you may come across, this is one you should really keep to heart (see what we did there?).
Want to have a healthy heart? The food you eat, and the quantity and quality of activity you choose to engage in can have a significant impact on the general health of your heart and the many other tissues that make up your cardiovascular system.
Controlling cholesterol is also crucial for heart health because it lowers your chances of heart disease, heart attack, and stroke. Low-density lipoprotein (LDL or “bad” cholesterol) and high-density lipoprotein (HDL or “good” cholesterol) are the two main types of cholesterol. Foods high in saturated fat, particularly animal proteins, include LDL cholesterol. Unless you want to have serious heart disease or heart attack, you should definitely avoid that!
Learn more about this vital organ with our comprehensive collection of 50 facts about the heart. We discuss treatments for heart disease, cuisines that have animal hearts, and a whole lot more!
- A human’s heart typically measures about the same size as their closed fist.
- A heart at rest usually beats 72 times per minute.
- Exercise causes temporary increases in heartbeat, while also lowering the resting heartbeat.
- Heart disease causes an estimated 30% of all deaths worldwide.
- A heart has 4 internal chambers, 2 aortas on top, and 2 ventricles below.
- Greek physician Hippocrates first observed blood passing through the heart to and from the lungs.
- Greek physician and anatomist Erasistratos discovered the heart’s valves, and how the heart acted as a pump for blood.
- Both Plato and Aristotle later believed that the heart also produced blood.
- Famous physician Galen differentiated venous and arterial blood from each other.
- 16th-century Flemish anatomist and physician Andreas Vesalius challenged the ancient Greek teachings about the heart following his own dissections in the 16th century.
- English physician William Harvey’s studies on the heart in the 17th century led to the medical community accepting Galen’s mistakes.
- Otto Frank and Ernest Starling discovered the Frank-Starling Law in the 19th Century.
- Sunao Tawara made breakthroughs in studying the heart’s electrical mechanisms in 1906.
- Heart disease became the most common cause of death in the USA from the 1950s onward.
- South African Surgeon Christiaan Barnard made the first heart transplant in 1967.
- Coronary Artery Disease (CAD) and strokes make up over 75% of all heart diseases.
- The term coronary comes from the Latin word for heart, cor.
- Doctors who specialize in the heart call themselves cardiologists.
- The name comes from the Greek word for heart, kardía (καρδία).
- Fish hearts only have 1 atrium and ventricle each, while reptile hearts have 3 chambers.
Blood comes to and from the heart in a fixed course.
Blood low in oxygen enters the heart through two veins, the superior and inferior venae cavae. Superior and inferior don’t actually mean better or poorer, as much as it does, upper and lower. Blood from both veins fills the right atrium, before getting pumped into the right ventricle. From there, it gets pumped into the pulmonary arteries, which take the blood to the lungs to get oxygenated. The now oxygen-rich blood returns to the heart through the pulmonary veins, into the left atrium. As the heart beats, it sends the blood into the left ventricle, from where it gets pumped through the aorta to the rest of the body.
The heart doesn’t sit in the exact center of the chest.
It’s actually oriented slightly to the left of the exact center of the chest. This comes from the fact that the left side of the heart has stronger muscles than the rest of the organ. This, in turn, developed from the fact that the left side of the heart sends blood not just to the lungs, but to the rest of the body. As such, it needs to have stronger muscles than the rest of the heart. That said, some people have a rare condition called dextrocardia, where the heart gets oriented towards the right side of the chest. They don’t usually suffer from the condition, but some become more vulnerable to cardiovascular, pulmonary, and intestinal disorders.
The heart has a skeleton of its own.
It isn’t made from bone or even cartilage, though. Instead, dense, fibrous tissues make up the heart’s skeleton, giving the organ its distinct shape. The skeleton also doubles as a non-conductive barrier to manage the heart’s electrical pulses. In particular, the rich collagen in the cardiac skeleton absorbs electricity, keeping it from going to where it’s not supposed to go.
Two different kinds of cells make up the heart’s muscles.
Muscle cells make up 99% of the heart, given its purpose to constantly pump blood to and from the rest of the body. Specialized pacemaker cells make up the remaining 1%, generating the electrical pulses that time the heart’s beating. Pacemaker cells actually have similarities to nerve cells, given their purpose. The heart’s muscle cells also have their own specialization, unique compared to the rest of the body’s muscles. Specifically, autorhythmicity, the ability to act at a fixed rate, as electrical impulses spread from one cell to the next.
The heart’s electrical current follows a specific path.
The Sino-Atrial (SA) Node generates the heart’s electrical currents, located along the heart’s right atrium. How it actually travels through the heart remains a mystery to medical science up to today. However, doctors do know the path it follows. From the right atrium, the electricity goes through Bachmann’s Bundle and into the left atrium. This causes both atriums to contract at the same time.
The electricity then passes through the atrioventricular septum between the right atrium and the left ventricle. From there, it passes through the Bundle of His (BH) and the Tawara Branches to the ventricles. Purkinje Fibers in both ventricles help distribute the electrical current to the heart’s muscles in the area.
A special sac surrounds the heart.
Doctors call it the pericardium, made up of inner and outer layers. A fibrous membrane makes up the tough outer layer, while a double-layer serous membrane makes up the inner layer. The serous membrane also produces pericardial fluid, which works as a lubricant for the heart.
The pericardium serves three purposes: first, to keep the heart from chafing against surrounding organs. Second, to stabilize the heart’s position in the chest, and finally, to protect the heart against infection.
The heart has two different nerves.
There’s the vagus nerve, which links directly to the brainstem, and another series of nerves connected to the sympathetic trunk. Both nerves don’t actually control the heartbeat, but influence it depending on the state of the rest of the body. In particular, signals from the vagus nerve work to decrease the heartbeat. In contrast, signals from the sympathetic trunk work to increase the heartbeat.
The heart becomes the first organ to finish forming.
In fact, the heart becomes fully functional even before an embryo grows into a fetus. This can happen as early as only 3 weeks into a pregnancy. Before birth, embryonic and fetal hearts have a small hole between the left and right atriums. This allows blood to bypass the lungs, as embryos and fetuses depend on their mother for oxygen. After birth, though, the heart automatically closes the hole and begins normal operations.
Cardiac Output (CO) refers to the amount of blood pumped by the heart every minute.
On average, an adult human’s heart pumps around 5.25 liters of blood every minute. The exact figure varies from person to person, though, from as low as 4 liters per minute, to as high as 8 liters per minute. Doctors measure a person’s CO first by getting the stroke volume (SV), or the amount of blood pumped by each ventricle. They then multiply it by heart rate, measured by the minute.
Age affects how many times a heart beats in a single minute.
Embryos and fetuses start out with a heartbeat similar to their mother’s, before accelerating up to 185 beats per minute around the seventh week of pregnancy. Around the ninth week, it decelerates, to around 145 beats per minute by the time of birth. It drops further after birth, to around 129 beats per minute, and continues to decelerate as the child grows. Adults typically average between 60 and 100 beats per minute.
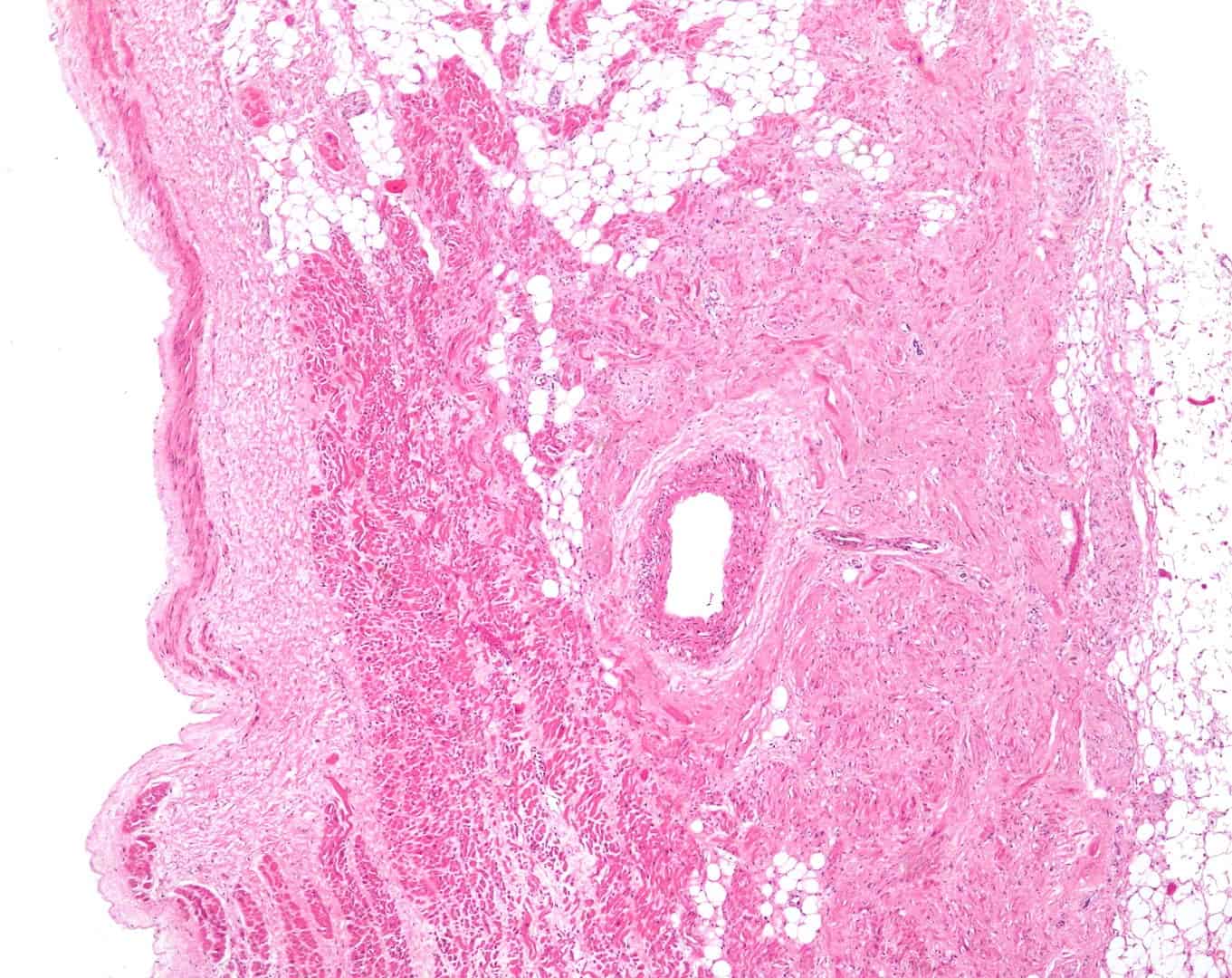
CAD results from atherosclerosis.
Atherosclerosis refers to the build-up of fatty deposits called plaques inside a person’s arteries. These plaques make the arteries narrower, and make it harder for blood to flow through them. That said, the heart and the body can cope with minor narrowing of the arteries. However, if they get too narrow, CAD results, with the potentially fatal symptom of heart attacks.
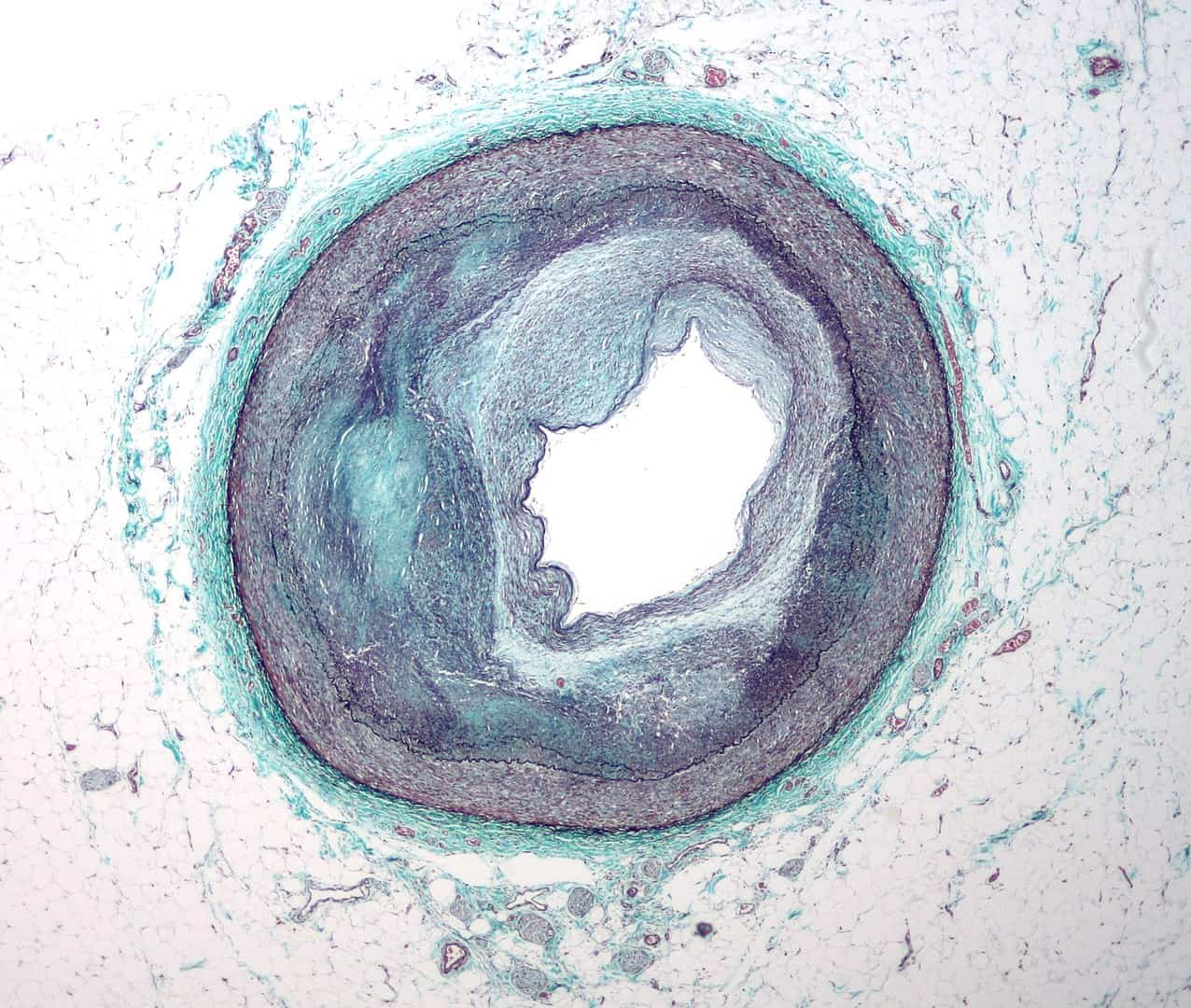
Various factors can lead to heart failure.
Obesity and high blood pressure make up the most common factors leading to heart failure. They don’t directly cause heart failure, instead causing conditions like CAD that can then lead to heart failure. Other conditions and factors that can lead to heart failure include diabetes, hypertension, high blood cholesterol, and even smoking.
Various diseases can also directly affect the heart’s muscles.
Doctors collectively call these diseases cardiomyopathies, which can affect the heart’s muscles in various ways. Hypertrophic cardiomyopathy, for example, causes an abnormal thickening of the heart’s muscles. This makes them less responsive to the heart’s electrical pulses, and weakens the heart’s ability to pump blood. Dilated cardiomyopathy abnormally swells and weakens the heart, while restrictive cardiomyopathy stiffens the heart. These diseases most commonly result as a form of hereditary disease.
The heart’s valves can also develop diseases of their own.
Doctors collectively call these diseases valvular heart disease. These affect the heart’s valves in various ways. Stenotic valve disease, for example, opens too narrowly and makes it difficult for blood to pass through the heart. Valvular regurgitation, in contrast, makes the valves malfunction so much so that they cause blood flow to actually flow in reverse. These diseases have various causes, most commonly resulting from old age, as well as from other conditions like rheumatism.
Arrhythmia causes the heart to beat irregularly.
Arrhythmia has many symptoms, with heart palpitations as the most common. Other symptoms include blackouts, with the most serious including heart failure and even stroke.
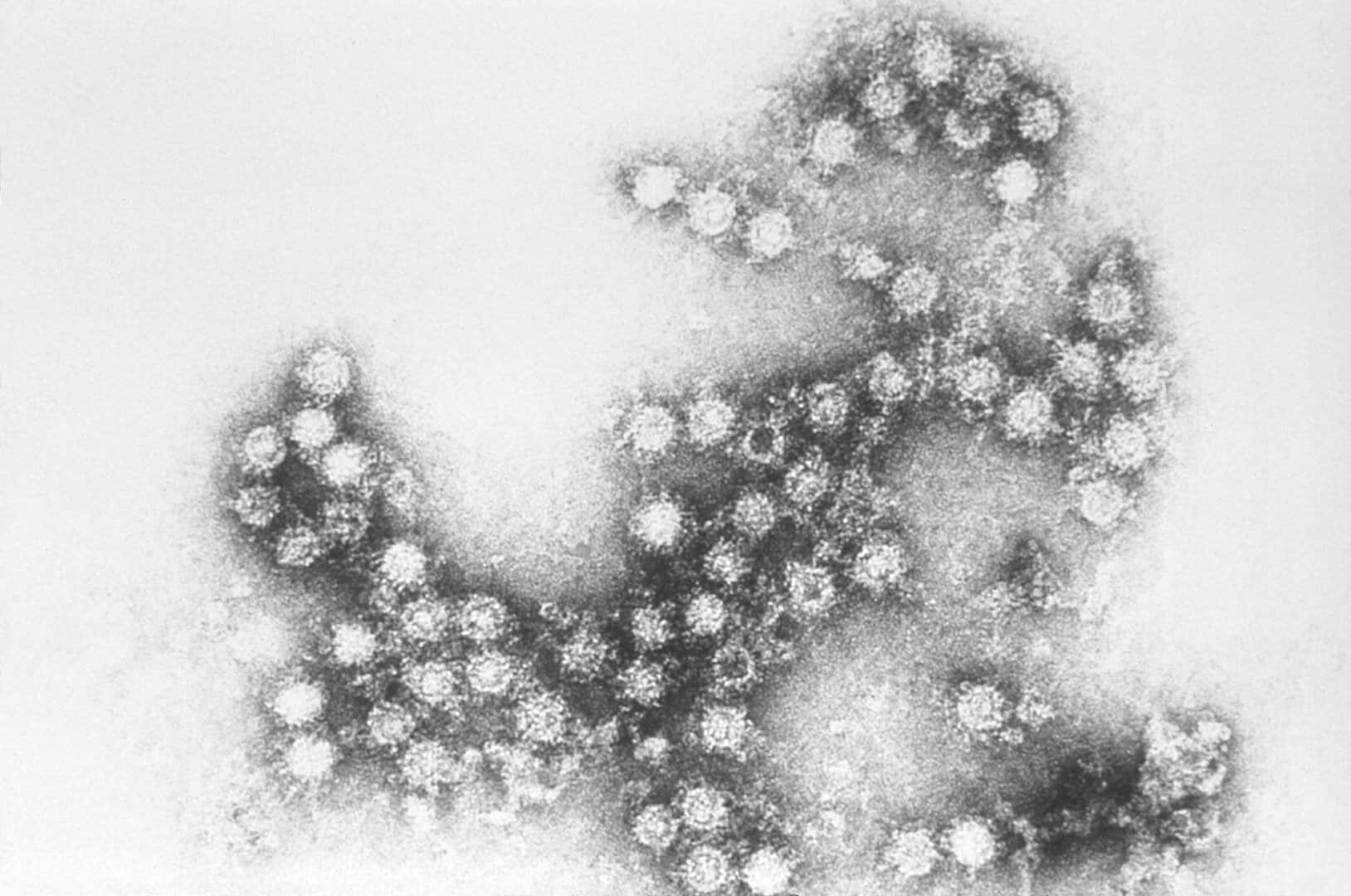
The pericardium can also develop diseases of its own.
Doctors collectively call these diseases pericarditis and typically cause the pericardium to become swollen. Viruses usually cause these diseases, such as Cytomegalovirus, Coxsackievirus, and the Epstein-Barr virus. These diseases commonly cause fluid to build up inside the pericardium, which then presses down on the heart. This results in low blood pressure, and which may become fatal.
Some people find themselves born with defective hearts.
Doctors prefer to use the professional term “congenital heart defects,” though. Minor ones include “patent foramen ovale,” where the hole between the atriums from before birth don’t properly close. A major example of a congenital heart defect includes hypoplastic left heart syndrome, where the left side of the heart suffers from various states of poor development. Those include an undersized atrium or ventricle, overly narrow valves, or simply no valves at all.
People can actually die from a broken heart.
Normally, we associate the term “dying from a broken heart,” with common cliches in television or radio soap operas. Medical professionals, though, recognize it as a rare, but very dangerous condition. In particular, it affects people suffering from especially severe depression, such as that caused by a recent loss of a loved one. In such a state, the body produces depressive hormones that can actually weaken and even stop the heart from beating. The person literally dies from a broken heart, much like what happens in fiction.
Heart cancer happens very rarely.
This comes from the fact that cancer basically involves the body’s cells multiplying out of control. However, heart cells only have a limited ability to multiply, or even to self-repair. While this can become a problem should the heart get injured, it also means the heart can only rarely if ever develop cancer of its own.
Doctors have many methods to check the heart’s condition.
The simplest method involves simply feeling for the heartbeat with their bare hand, or with a stethoscope. Checking for the pulse, whether at the neck or the wrist, also counts as a common way of checking the heart’s condition. More complex methods include measuring blood pressure or using an electrocardiograph to measure the heart’s electrical impulses.
Invasive methods to actually see the heart also exist, usually using a small camera mounted at the end of a very thin wire inserted through a small hole in the chest. Noninvasive methods also exist, such as ultrasound, Computer Tomography (CT) scanning, Magnetic Resonance Imaging (MRI), and Positron Emission Tomography (PET).
Some types of heart disease don’t have symptoms.
This particularly proves the case with arrhythmia, with the body simply adapting to minor irregularities in the heartbeat. Patients can live completely normal lives, only needing to consult the doctor every once in a while just to make sure that their condition isn’t getting worse over time.
Some diseases can actually make heart disease more likely to develop.
Cardiomyopathy, for example, can also result from conditions such as alcoholism or drug abuse. Strep throat and endocarditis can also cause valvular heart disease as additional complications on top of their other symptoms. In addition to viral infections, pericarditis can also result from other conditions, such as cancer and kidney failure.
They also have various treatments for the heart’s diseases.
Some of the simplest treatments include drugs Nitroglycerin for CAD, and even Aspirin, to reduce the risk of strokes. Many other drugs exist for more serious conditions, such as calcium or sodium channel blockers for people with severe arrhythmia. For the most serious cases, doctors use surgery to widen arteries, or even bypass blocked sections entirely, the so-called heart bypass surgery. Other surgical procedures on the heart include replacing defective valves with artificial valves.
Pacemakers can help regulate a heart’s beating.
These implants measure only as big as a Matchbox car, but they’ve saved the lives of millions of people around the world. In fact, up to 600,000 people per year find themselves implanted with a pacemaker. Doctors use these amazing machines to regulate hearts that can no longer regulate themselves. Implanted right next to a heart, a pacemaker generates the proper electrical impulses needed to keep a heart beating properly.
First developed in 1926, research continued through the following decades, with external pacemakers entering medical service in 1958. Development on internal pacemakers began the following year, and entered medical service in the 1960s.

Heart transplants make for risky operations.
So much so, that doctors consider them the last resort when it comes to keeping patients with heart problems alive. This comes from the fact that even with a healthy donor with a matching blood type, the patient’s body will eventually reject a transplanted organ. This forces patients to take anti-rejection drugs, but those work by suppressing the body’s immune system, leaving them vulnerable to injection.
Doctors expected the problem as early as the first heart transplant in 1967. But even then, they couldn’t stop their patient, Louis Washkansky, from contracting and then dying from pneumonia just 18 days afterward. This forces doctors and patients alike to maintain constant monitoring to minimize the risk of both rejection and infection.
Prevention remains the best solution for heart disease.
Something as simple as stopping smoking, avoiding drugs, and drinking in moderation can go a long way to keeping your heart healthy. An active lifestyle with plenty of exercises and a healthy diet also does wonders for the heart. In fact, doctors prefer not letting a heart condition develop in the first place over having to prescribe a cure after it develops.
The heart has long had powerful symbolism in religion and culture worldwide.
As far back as in ancient times, even. The Ancient Egyptians believed that the god Anubis tested the hearts of the dead for their worthiness to enter the afterlife. Furthermore, Abrahamic traditions associate the heart with the Throne of God, which later led to the veneration of the Heart of Christ. In Hinduism and Taoism, the heart served as the source of wisdom and understanding. Greco-Roman scholars saw the heart as the source of thought and reason, going so far as to ignore all evidence that pointed to the brain instead. In Mesoamerica, the natives saw the heart as the source of all life, holding inside a fragment of the Sun’s fire. This led to the practice of offering the hearts of living sacrifices to the Sun as part of their religion.
Some cuisines feature animal hearts as an ingredient.
Nutrition-wise, hearts have rich protein content, while its nature as a muscular organ makes for firm and dry meat. This typically leads to slow cooking for dishes that feature heart meat, and which usually include other organs in the recipe. Hearts may also cook by grilling, such as in dishes like the Brazilian churrasco de curacao, Indonesian chicken heart satay, and Japanese hatto yakitori.

Not all animals have hearts.
Worms, for example, don’t need blood as they directly absorb oxygen into their bodies from a series of connected tubes. Insects and mollusks also lack proper hearts, instead having a separate muscle that runs the length of their bodies. This muscle keeps their blood moving to and from a separate cavity called the hemocoel and a series of connected tubes.
Mammals and birds share the same heart design.
Birds inherited a four-chambered heart design from their dinosaur ancestors, who evolved into a four-chambered heart out of necessity given their large bodies. Mammals developed a four-chambered heart similarly, in what scientists call parallel evolution. Mammals and birds also share a distinction that both make up the only warm-blooded vertebrates. This has led scientists to consider the theory that only warm-blooded animals have four-chambered hearts.
Was this page helpful?
Our commitment to delivering trustworthy and engaging content is at the heart of what we do. Each fact on our site is contributed by real users like you, bringing a wealth of diverse insights and information. To ensure the highest standards of accuracy and reliability, our dedicated editors meticulously review each submission. This process guarantees that the facts we share are not only fascinating but also credible. Trust in our commitment to quality and authenticity as you explore and learn with us.


