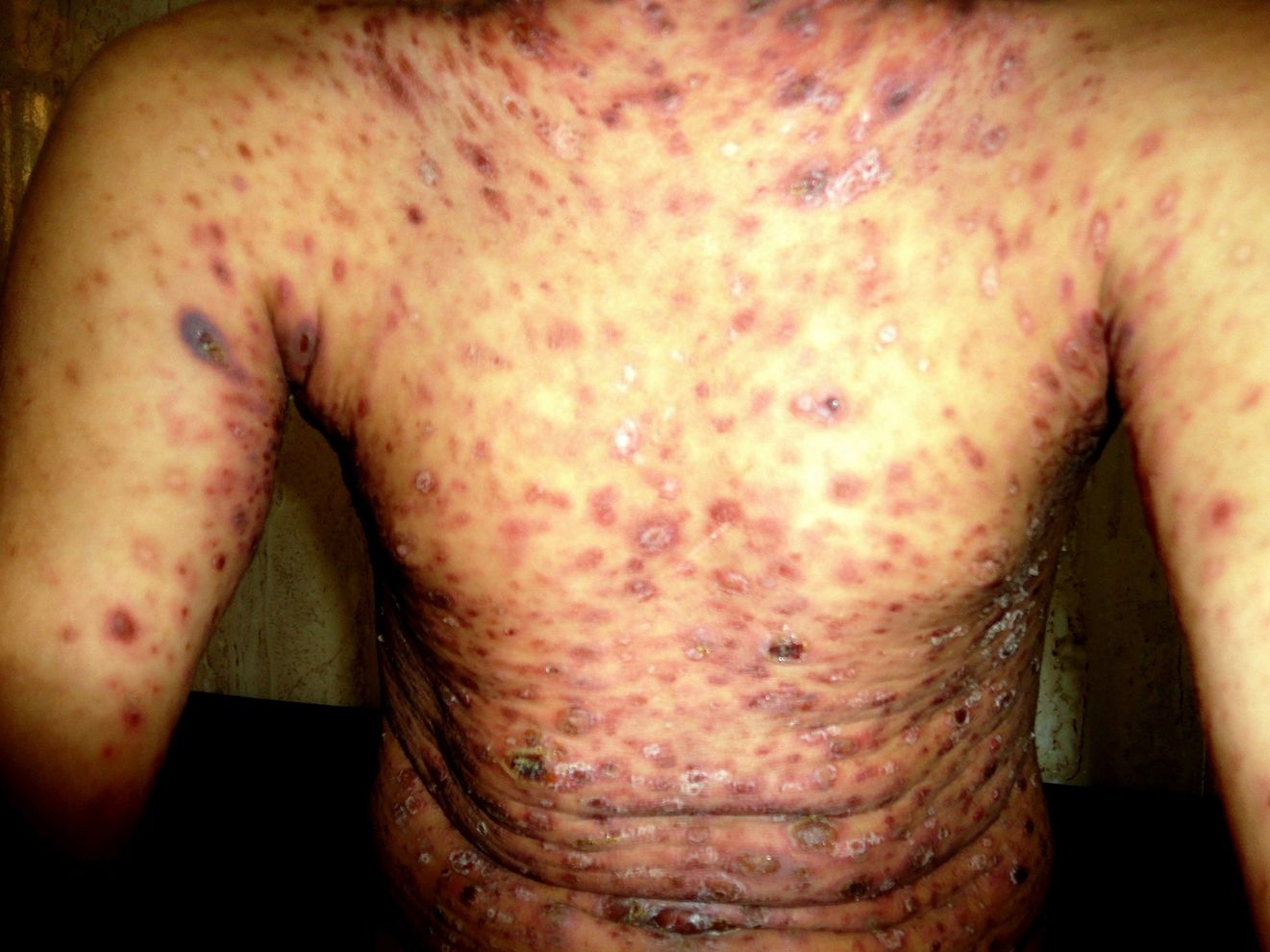
Mucha–Habermann disease, also known as pityriasis lichenoides et varioliformis acuta (PLEVA), is a rare skin disorder that can be quite puzzling. It often starts with red spots that turn into blisters or crusty sores. These lesions can appear suddenly and might leave scars. The exact cause remains unknown, but it’s believed to involve an abnormal immune response. This condition affects both children and adults, though it’s more common in young people. Treatment varies, ranging from antibiotics to phototherapy. Understanding Mucha–Habermann disease can help manage symptoms and improve quality of life for those affected.
Key Takeaways:
- Mucha–Habermann Disease, also known as PLEVA, causes red, scaly patches that can turn into blisters. It's most common in children and young adults, and there's no known cure.
- Managing Mucha–Habermann Disease involves treatments like corticosteroids and antibiotics, as well as lifestyle adjustments and regular follow-ups with a dermatologist. Support groups and education can also help cope with the condition.
What is Mucha–Habermann Disease?
Mucha–Habermann disease, also known as pityriasis lichenoides et varioliformis acuta (PLEVA), is a rare skin disorder. It presents with red, scaly patches that can turn into blisters or ulcers. Understanding this condition can help in managing its symptoms better.
- Mucha–Habermann disease is named after two dermatologists, Rudolf Mucha and Robert Habermann, who first described it in the early 20th century.
- This disease is part of a spectrum of disorders known as pityriasis lichenoides.
- PLEVA can affect individuals of any age but is most commonly seen in children and young adults.
- The exact cause of Mucha–Habermann disease remains unknown.
- Some researchers believe it may be linked to an immune system reaction.
Symptoms of Mucha–Habermann Disease
Recognizing the symptoms is crucial for early diagnosis and treatment. The disease manifests in various ways, often making it challenging to identify.
- Red, scaly patches are the most common symptom.
- These patches can evolve into blisters or ulcers.
- The lesions often appear in clusters.
- They can be itchy or painful.
- In some cases, the disease can cause fever and malaise.
Diagnosis of Mucha–Habermann Disease
Diagnosing Mucha–Habermann disease involves a combination of clinical evaluation and laboratory tests. Dermatologists play a key role in identifying this condition.
- A skin biopsy is often required to confirm the diagnosis.
- The biopsy typically shows inflammation and necrosis of the skin.
- Blood tests may be conducted to rule out other infections or autoimmune disorders.
- Dermoscopy, a non-invasive skin imaging technique, can help in visualizing the lesions.
- Sometimes, a differential diagnosis is necessary to distinguish it from other skin conditions like psoriasis or eczema.
Treatment Options for Mucha–Habermann Disease
While there is no cure for Mucha–Habermann disease, several treatments can help manage the symptoms and improve the quality of life for those affected.
- Topical corticosteroids are commonly prescribed to reduce inflammation.
- Antibiotics like tetracycline can be effective in some cases.
- Phototherapy using ultraviolet light may help clear the lesions.
- Immunosuppressive drugs are sometimes used for severe cases.
- Oral corticosteroids can be prescribed for short-term relief.
Living with Mucha–Habermann Disease
Managing Mucha–Habermann disease involves more than just medical treatments. Lifestyle adjustments and support systems play a significant role in coping with the condition.
- Regular follow-ups with a dermatologist are essential.
- Moisturizing the skin can help alleviate dryness and itching.
- Avoiding triggers like stress and certain foods may reduce flare-ups.
- Support groups can provide emotional and psychological support.
- Education and awareness about the disease can empower patients and their families.
Final Thoughts on Mucha-Habermann Disease
Mucha-Habermann Disease, or Pityriasis Lichenoides et Varioliformis Acuta (PLEVA), is a rare skin condition that can be challenging to diagnose and treat. Symptoms include red, scaly patches and lesions that can be painful or itchy. While the exact cause remains unknown, some believe it might be linked to immune system issues or infections. Treatments vary from antibiotics to phototherapy, depending on severity. Early diagnosis and proper management can significantly improve quality of life for those affected. If you or someone you know shows symptoms, consult a healthcare professional for accurate diagnosis and treatment options. Staying informed and proactive can make a big difference in managing this condition.
Frequently Asked Questions
Was this page helpful?
Our commitment to delivering trustworthy and engaging content is at the heart of what we do. Each fact on our site is contributed by real users like you, bringing a wealth of diverse insights and information. To ensure the highest standards of accuracy and reliability, our dedicated editors meticulously review each submission. This process guarantees that the facts we share are not only fascinating but also credible. Trust in our commitment to quality and authenticity as you explore and learn with us.
